Stress, Anxiety, Depression & OCD Treatment

Comprehensive Psychiatric Care in the Indian Context
Mental health concerns such as stress, anxiety, depression, and OCD are extremely common in India — yet many people suffer silently.
As a leading psychiatrist in the city, I often see patients who have been struggling for months or even years before seeking help. Most did not recognise their symptoms as mental health concerns. Many believed it was “just stress.”
Early understanding and timely treatment can prevent long-term suffering.
Understanding Mental Health in the Indian Context
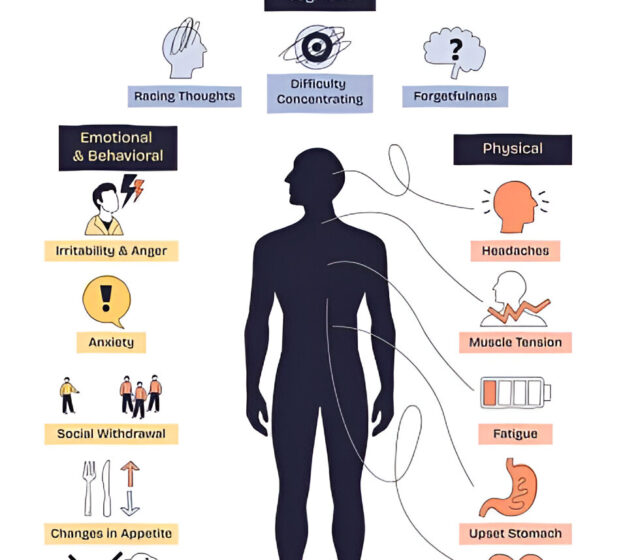
In India, emotional distress often presents differently from textbook descriptions. Because of:
- Cultural beliefs
- Family expectations
- Academic and career pressure
- Marital and relationship stress
- Financial responsibilities
- Social stigma
Many individuals do not say, “I am depressed” or “I am anxious.” Instead, they report:
- बिना कारण शरीर में दर्द expectations
- सिर में भारीपन
- नींद न आना
- दिल की धड़कन तेज होना
- हर समय थकान महसूस होना
- कमजोरी और थकावट
Stress: When Does It Become a Disorder?
Stress is normal. But chronic stress can gradually develop into anxiety and depression. Common Indian triggers:
- High academic expectations expectations
- Long working hours
- Caregiving for elderly parents
- Marital conflicts
- Urban loneliness
- Competitive work culture
Warning signs stress is becoming harmful:
- Irritability
- Sleep disturbance
- Loss of motivation
- Frequent headaches
- Constant worrying
- Reduced concentration
Early psychiatric guidance prevents progression.
Anxiety Disorders (चिंता और घबराहट)
Anxiety becomes a disorder when worry is excessive, persistent, and uncontrollable.
Common symptoms:
ज्यादा सोचने की आदत
मन बेचैन रहना
घबराहट के दौरे
Restlessness
Palpitations
Sweating
Sleep disturbance
Fear without clear reason (बेवजह डर लगना)
Types of anxiety disorders include:
Generalised Anxiety Disorder
Panic Disorder
Social Anxiety
Health Anxiety
Untreated anxiety affects work performance, relationships, and physical health.
Anxiety Disorders (चिंता और घबराहट)
Obsessive Compulsive Disorder (OCD)
Depression is not just sadness.
It may present as:
उदासी और मन भारी रहना
निराशा और खालीपन
किसी काम में मन न लगना
Fatigue
Sleep changes
Appetite changes
Emotional numbness
Irritability
Reduced productivity
Many patients continue functioning outwardly while suffering internally.
High-functioning depression is common in professionals and homemakers.
OCD involves unwanted repetitive thoughts (obsessions) and repetitive behaviours (compulsions).
Common examples:
Repeated hand washing
Checking locks multiple times
Excessive cleaning
Fear of contamination
Intrusive disturbing thoughts
Need for symmetry or exactness
Patients usually know the thoughts are irrational but feel unable to control them.
OCD is treatable with therapy and medication.
Other Neurotic Disorders
Neurotic disorders include conditions where individuals remain in touch with reality but experience significant distress.
These include:
Phobias
Health anxiety
Somatic symptom disorders
Adjustment disorders

Stress-related sleep disorders
Why Many People Delay Psychiatric Treatment
Common beliefs:
- “This is just stress.”
- “Everyone feels like this.”
- “I am physically unwell, not mentally.”
- “Psychiatric medicines are addictive.”
- “Only severe cases need a psychiatrist.”
By the time help is sought, symptoms may have become chronic.
Somatic Symptoms: When the Body Speaks
In Indian clinical practice, emotional distress often appears as physical symptoms.
Common presentations:
- बिना कारण शरीर में दर्द
- सिर में भारीपन
- Gastrointestinal discomfort
- Chest tightness
Chronic fatigue - Multiple normal medical reports
How Psychiatric Treatment Helps
Comprehensive Evaluation
We assess:
- Emotional symptoms
- Stressors
- Physical health
- Family context
- Personality factors
Correct diagnosis ensures appropriate treatment.
Medication (When Required)
Not all patients need medication.
- Medicines are evidence-based
- Doses are carefully monitored
- Follow-up is regular
- Safety is prioritised
Most antidepressants are not addictive.
Psychotherapy
Therapy helps patients:
- Manage stress
- Control negative thoughts
- Reduce compulsive behaviours
- Improve coping skills
- Develop emotional resilience
For OCD, specialised therapy is highly effective.
Lifestyle & Stress Regulation
Treatment also focuses on:
- Sleep hygiene
- Work-life balance
- Digital detox
- Exercise
- Structured routines
Mental health recovery is holistic.
Frequently Asked Questions (FAQs)
“How do I know if I have depression?”
If low mood, loss of interest, or fatigue persist for more than two weeks and affect functioning, evaluation is recommended.
“Are psychiatric medicines addictive?”
Most antidepressants and anti-anxiety medications are not addictive when prescribed appropriately.
“Can anxiety go away on its own?”
Mild stress may improve.
Persistent anxiety usually requires structured intervention.
“Is OCD curable?”
OCD can be effectively managed with medication and therapy. Many patients lead completely normal lives.
“If I am working normally, can I still have depression?”
Yes. Many individuals function externally while suffering internally.
“Will people know if I consult a psychiatrist?”
Consultations are confidential.
“How long does treatment take?”
Mild cases may improve within weeks.
Moderate to severe cases require structured follow-up for several months.
Consistency improves outcome.
The Risk of Partial Treatment
Many patients:
- Continue the same antidepressant for years without review
- Receive symptom-based treatment without diagnosis
- Focus only on physical tests
Without proper assessment and follow-up, recovery may remain incomplete.
Structured psychiatric care prevents unnecessary long-term medication exposure.
Why Early Intervention Matters
Early psychiatric care:
- Prevents worsening of symptoms
- Reduces risk of substance misuse
- Improves work productivity
- Strengthens family relationships
- Enhances quality of life
Mental health conditions are treatable medical disorders — not personality flaws.
Our Approach to Stress, Anxiety, Depression & OCD
We provide:
- Detailed psychiatric assessment
- Evidence-based diagnosis
- Personalised treatment planning
- Medication management when required
- Psychotherapy integration
- Regular follow-up
- Confidential and respectful care
Each patient receives individualised attention.
When Should You Consult a Psychiatrist?
Seek consultation if you experience:
- Persistent sadness or irritability
- Constant worry
- Panic attacks
- Repetitive intrusive thoughts
- Sleep disturbance
- Physical symptoms without clear cause
- Reduced work efficiency
- Loss of interest in life
If symptoms affect your daily functioning, do not delay.
Breaking Common Myths

Myth: “Depression is weakness.”
Fact: It is a medical condition.
Myth: “Medicines change personality.”
Fact: Proper treatment restores natural personality.
Myth: “Talking about stress makes it worse.”
Fact: Early discussion reduces severity.
Myth: “Only severe mental illness needs treatment.”
Fact: Early care prevents chronic illness.
Take the First Step Toward Mental Wellness
Stress, anxiety, depression, and OCD are common and treatable.
Seeking help is not weakness.
It is a responsible decision toward better health.
Timely psychiatric care can restore balance, productivity, and emotional stability.
